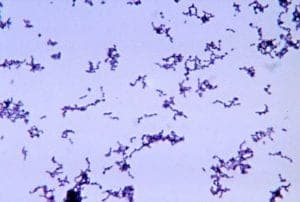
For years, it was believed that an excess of a bacterium called Propionibacterium acnes (P. acnes) on the skin contributed to acne.
But researchers have now found it’s rather the imbalance of this bacterium on the skin that causes acne, according to a study published in the journal Scientific Reports.
A popular method of treating acne among dermatologists has been to prescribe antibiotics in addition to some topical treatment. However, antibiotics kill off all the bacteria — including the good kind. The UCLA researchers involved in the study suggest that balancing bacteria on the skin may be the way of the future in battling acne breakouts.
The researchers gathered cleansing pore strips to collect DNA from 38 adults with acne and 34 adults without. The DNA was then used to analyze and compare the bacterial makeup of the two groups.
“This allowed us to look not only at what species of bacteria were there, but also at their genomic content to see what kinds of genes they had,” said study author Dr. Huiying Li, an associate professor of Molecular and Medical Pharmacology at the David Geffen School of Medicine at UCLA.
Related: Try These 7 Foods for Healthy, Glowing Skin
Both groups had P. acnes strains on their skin, but in the acne-free group the skin microbiome had genes related to bacterial metabolism, a processes that is believed to prevent harmful bacteria from growing.
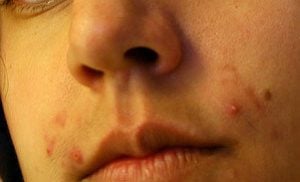
However, the group of participants with acne had higher levels of a gene which produces and transports bacterial toxins and other pro-inflammatory compounds.
“You may have the bad bacteria, but if you also have good ones in the same community that can counterbalance the bad guys, you may not have acne,” Li said.
With about 85 percent accuracy, the researchers were able to tell if a person had acne based just on their bacterial makeup. Although the study’s sample size was small, the results were the same when the researchers tested another 10 volunteers.
Related: Acne-Causing Bacteria Might Also Fight Skin Disease
More research is still needed, but the study authors suggest that balancing the skin’s microbiome may be a better, more effective way of treating acne than antibiotics, which in the long term can lead to antibiotic resistance.
“Everybody has P. acnes, and some P. acnes are good, in general, for our skin,” Li said. “We need to figure out how to selectively get rid of the bad ones but keep the good.”
Danielle Tarasiuk is a multimedia journalist based in Los Angeles. Her work has been published on AllDay.com, Yahoo! Sports, KCET, and NPR-affiliate stations KPCC and KCRW. She’s a proud Sarah Lawrence College and USC Annenberg alumn.


![How To: ‘Fix’ Crepey Skin [Watch]](https://cdn.vitalupdates.com/wp-content/uploads/2017/05/bhmdad.png)












