A readily available vaccine can wipe out nearly all cases of infection-linked cervical cancer, shows a new study from researchers in Australia.
Receiving a vaccine for human papillomavirus (HPV) can safely protect up to 93 percent of certain populations of women from developing cervical cancer, which affects nearly 13,000 women in the United States every year.
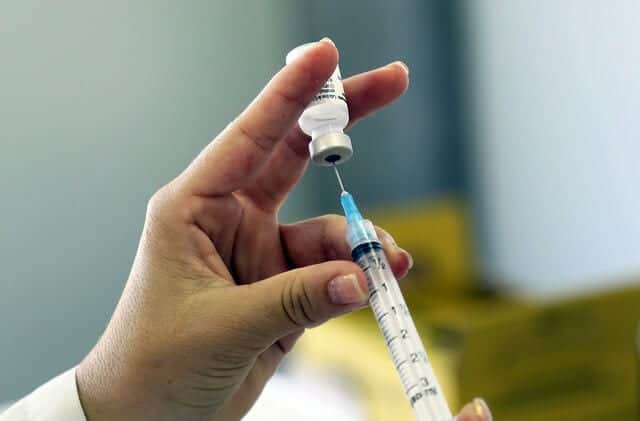
The new study, appearing in the International Journal of Cancer, looked specifically at Australian women and found that the currently available HPV vaccine (Gardasil) covers two of the most common strains of the virus.
The results are “great news for our daughters and all young Australian women,” said lead author Julia Brotherton, Medical Director of Australia’s National HPV Vaccination Program Register at Victorian Cytology Service.
More than 200 types of HPV exist, and about 40 strains of the virus are easily spread via sexual contact, notes the National Cancer Institute. The Gardasil vaccine covers two of the strains most commonly linked to cancer — strains 16 and 18 — and in Australia those strains make up about 77 percent of all HPV cases.
Internationally, the 16 and 18 strains remain two of the most prevalent strains, but at a slightly lower rate of 71 percent. Because the difference in incidence is small, Gardasil is highly effective in reducing the risk of cervical cancer among women around the globe.
New Vaccine Is Even Better
But there’s even better news on the horizon, according to the Australian researchers, who point to a new vaccine, currently under the consideration of Australia’s national health center, that would prevent the infection of five additional strains of HPV (strains 31, 33, 45, 52 and 58).
“This study highlights that the new HPV vaccine yet to be released in Australia could prevent over 90 percent of cervical cancers, which is an incredibly exciting prospect,” said Brotherton.
Current recommendations from the Centers for Disease Control and Prevention (CDC) call for all children — both boys and girls — to get the HPV vaccine at ages 11 or 12. At that age, two shots are required. When a child is older than 12, a course of three shots will be necessary, says the CDC.
Related: Clinical Trials for Type 1 Diabetes Vaccine Coming Soon
More than 80 million people currently carry one form of HPV or another, and about 14 million teenagers will acquire the virus in a given year. While most cases of HPV go away on their own, some infections last longer, eventually leading to dangerous outcomes, including cancers of the cervix, vagina and vulva. The virus can also lead to penis cancer in men, as well as cancers of the anus and throat in both men and women.
“The biggest message is: we must have high coverage of the vaccine to prevent the HPV infection that causes cervical cancer,” said senior author Suzanne Garland, Director of the Royal Women’s Hospital Centre for Infectious Diseases.
Should more individuals gain coverage, the threat of cervical cancer among women would be severely diminished.
“The new vaccine still protects against genital warts but is expanded to cover the seven most common viral types that cause cervical cancer. I do believe that if we continue with this high coverage of vaccination, we could almost wipe out cervical cancer in women,” said Garland.
Richard Scott is a health care reporter focusing on health policy and public health. Richard keeps tabs on national health trends from his Philadelphia location and is an active member of the Association of Health Care Journalists.


![How To: ‘Fix’ Crepey Skin [Watch]](https://cdn.vitalupdates.com/wp-content/uploads/2017/05/bhmdad.png)












