Gonorrhea, a sexually transmitted disease that affects more than 78 million people a year, is becoming impossible to treat.
The World Health Organization announced that the disease is becoming resistant to a wide range of antibiotics, making it nearly untreatable.
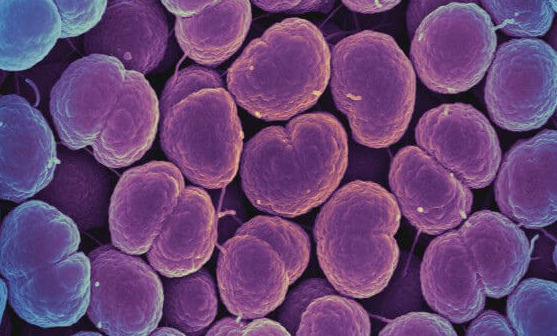
“The bacteria that cause gonorrhoea are particularly smart. Every time we use a new class of antibiotics to treat the infection, the bacteria evolve to resist them,” said Teodora Wi, a medical officer for the WHO Department of Reproductive Health.
Resistance to antibiotics makes the disease extremely hard to control and manage, said a study led by Wi. The study calls for international collaborative action to tackle the growing need for new treatments to combat gonorrhoea.
Another study said the disease isn’t resisting just one antibiotic, but all of them. And the antibiotics that do manage to treat the disease are also “under threat.”
“Almost all antibiotic classes used against gonorrhoea lost their efficacy because of resistance,” the study said. “Sulfononamides, penicillins, early-generation cephalosporins, tetracyclines, macrolides and fluoroquinolones can no longer be relied upon. The extended-spectrum cephalosporins, which represent the last remaining option for first-line empirical monotherapy, are also under threat with resistance reported worldwide.”
Related: Regular Sexual Activity Could Improve Cognitive Function in Older Adults
Even high-income countries with state-of-the-art healthcare are facing cases of gonorrhea that have become resistant to treatment via any known antibiotics. Wi said the higher-income countries could be just the beginning for understanding the need for different treatments.
“These cases may just be the tip of the iceberg, since systems to diagnose and report untreatable infections are lacking in lower-income countries where gonorrhoea is actually more common,” she said.
There are currently only three new candidate drug treatments undergoing clinical development, but they don’t appeal to many pharmaceutical companies because the drugs are only taken for a short amount of time and resistance builds quickly. Manica Balasegaram, director for the Global Antibiotic Research and Development Partnership, said the nonprofit organization is working to advocate for better gonorrhea treatments.
Related: These 7 Foods Could Be Killing Your Sex Drive
“To address the pressing need for new treatments for gonorrhoea, we urgently need to seize the opportunities we have with existing drugs and candidates in the pipeline. In the short term, we aim to accelerate the development and introduction of at least one of these pipeline drugs, and will evaluate the possible development of combination treatments for public health use,” Balasegaram said. “Any new treatment developed should be accessible to everyone who needs it, while ensuring it’s used appropriately, so that drug resistance is slowed as much as possible.”
There aren’t any affordable rapid care diagnostic tests for gonorrhea and many affected are symptomless and unaware, the WHO said. In addition, doctors often assume a patient has gonorrhea without investigating further, prescribing unnecessary antibiotics that can lead to antibiotic resistance.
“To control gonorrhoea, we need new tools and systems for better prevention, treatment, earlier diagnosis, and more complete tracking and reporting of new infections, antibiotic use, resistance and treatment failures,” said Marc Sprenger, director of Antimicrobial Resistance at WHO. “Specifically, we need new antibiotics, as well as rapid, accurate, point-of-care diagnostic tests – ideally, ones that can predict which antibiotics will work on that particular infection – and longer term, a vaccine to prevent gonorrhoea.”
Tori Linville is a freelance writer and editor from Clarksville, Tennessee. When she isn’t writing or teaching, she’s faithfully watching her alma mater, the University of Alabama, dominate the football field.


![How To: ‘Fix’ Crepey Skin [Watch]](https://cdn.vitalupdates.com/wp-content/uploads/2017/05/bhmdad.png)












